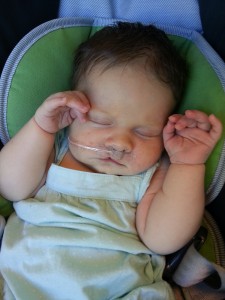
 Evie’s cleft lip was a birthday surprise. Though some parents are informed of their child’s cleft at the 20 week ultrasound, I saw it when she was laid in my arms for the first time (birth story to come)! I knew something was wrong with her lip right away, but I was just so relieved to be done laboring to care much at all. Within ten minutes of her birth, she was examined by a pediatrician who diagnosed her with a unilateral incomplete cleft lip (unilateral meaning it is only on one side, and incomplete meaning it does not extend all the way up into her nose). He determined she most likely did not have a cleft palate, and then left us with reading material all about clefts.
Evie’s cleft lip was a birthday surprise. Though some parents are informed of their child’s cleft at the 20 week ultrasound, I saw it when she was laid in my arms for the first time (birth story to come)! I knew something was wrong with her lip right away, but I was just so relieved to be done laboring to care much at all. Within ten minutes of her birth, she was examined by a pediatrician who diagnosed her with a unilateral incomplete cleft lip (unilateral meaning it is only on one side, and incomplete meaning it does not extend all the way up into her nose). He determined she most likely did not have a cleft palate, and then left us with reading material all about clefts.
When the pediatrician said she had a cleft lip, my absurdly naïve initial thought was “wait…I thought clefts were only a third world problem.” I guess I had this impression due to the “Operation Smile” commercials asking for donations for children in third world countries who need cleft repairs (I’m sure you’ve seen them), and because up until that point, I had never personally known anyone with a cleft. Obviously this isn’t the case 🙂 I later learned that clefts are actually the fourth most common birth defect, and 1/700 children are born with a cleft lip and/or palate.
Truthfully, the moment I received her diagnosis, I really wasn’t very concerned about it and felt at peace (although I haven’t always felt that way over the last few months). I’m sure this was partly due to the hospital staff’s promptness in educating us about it, and partly because she was already breastfeeding before I even had the opportunity to consider she might not be able to – so I never spent any time worrying about that. Ironically, she nurses WAY better than Caleb ever did…and he had no excuse!
The pediatrician told us she was going to need surgery at some point, but I tried not to dwell on that because I wanted to focus on being present in the moment and bonding with her – not stressing about the future. I wasn’t bothered by how the cleft made her look, and proudly announced her arrival to family and friends with a photo. I guess I’d like to think that physical appearance just doesn’t matter…she was and is beautiful to me inside and out, and I’m ok with how God made her. I mean, sure, I’ve had moments when I’ve wondered “why her?” or “did I do something to cause it?”, but I know that as far as medical problems go, a cleft lip is really pretty minor (especially hers).
When we got home from the hospital, I’m pretty sure I read every single internet resource on clefts to get informed (and then some). I learned that a child can be born with a cleft lip only, a cleft palate only, or both. Clefts occur when tissues in the baby’s face and mouth don’t form properly. Normally, the tissues that make up the lip and palate fuse together in the second and third months of pregnancy, but in babies with cleft lip and cleft palate, the fusion never takes place or occurs only partially, leaving an opening (cleft).
The goals of treatment for cleft lip and cleft palate are to ensure the child’s ability to eat, speak, hear, and breathe, and to achieve a normal facial appearance. Treatment involves surgery to repair the defect and therapies to improve any related conditions. Researchers believe that most cases of cleft lip and cleft palate are caused by an interaction of genetic and environmental factors, but in many babies, a definite cause isn’t discovered. Evie falls into this category because she defies every known association (no family history, Caucasian, female, no exposure to alcohol/drugs/smoke, I’m not obese, I don’t have diabetes, I didn’t take medicine while pregnant, and I took prenatal vitamins).
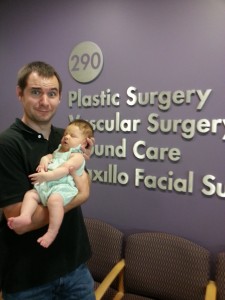
Our first week home from the hospital was fairly low-key, but life soon became filled with phone calls with Kaiser, doctor’s appointments, and pre-surgical treatments. We met with Evie’s plastic surgeon when she was just a week and a half old, and the appointment went really well. We thought Dr. Yokoo was very friendly, and took the time to answer each of our questions in-depth (she spent over an hour with us, which I think is a first in the history of all doctor’s appointments)! She has been doing cleft surgeries for a long time, and that boosted our confidence a lot. She thoroughly examined Evie’s mouth and confirmed that her palate was intact. We were so relieved to receive that news, because a cleft palate is really an entirely different animal requiring additional surgeries, and carries with it a host of likely complications including chronic ear infections, hearing loss, feeding difficulties, dental abnormalities, and lasting speech difficulties.
At the conclusion of our appointment with Dr. Yokoo, she took pictures of Evie and sent them to a orthodontist specializing in clefts for review. When the surgeon mentioned orthodontist, we were really confused as to why one would be involved (when I think orthodontist, I think teeth and braces). Two weeks later, we met with the orthodontist at Santa Clara Kaiser when Evie was 3 weeks old, and discovered it is because of a pre-surgical treatment called nasoalveolar molding (NAM) that is sometimes used with cleft infants, which utilizes orthodontic-like devices and is characterized by small adjustments to these devices over time.
NAM for babies with a cleft lip and/or palate is the fancy name given to the effort during the first few months of life to attempt to reduce the size of the gap in the mouth, stretch the lip muscles and bring the lip segments together, and to make the nose more symmetrical. This is supposed to be accomplished through the use of lip taping and a nose molding device. At our first appointment, the orthodontist gave us a power point presentation about NAM and showed us several before and after pictures depicting great results, so we were excited to go ahead with the treatment. He had us begin by doing lip taping only, which is a 5-10 minute procedure that must be repeated two to three times per day. Here’s what it entails: first, we use a q tip to apply medical adhesive (glue) onto her lip, next we cut a piece of medical tape to size, and lastly we lay the tape down on one side of her lip and squeeze her cleft together as we press it down across the other side. To remove the tape, we use another q tip with adhesive remover to get it off without ripping her skin.
At our next appointment with the orthodontist one week later, we added a nose molding device (see below) in addition to the lip taping, which in theory would push up on the cartilage of the flat side of her nose, gradually making her nostrils more symmetrical. This required us to first complete the taping routine described above, then apply more adhesive on top of the tape, attach a piece of floss to the nose molding device to prevent losing it since it’s so small, place the nose molding device *precisely* into her nose, apply more adhesive, apply another piece of tape to hold it in place, apply adhesive to her cheek, and apply another piece of tape to hold the floss down so she couldn’t pull the NAM device out. Whew! So with the NAM device added to the routine, it took about 15-20 minutes to complete and required two people…one to hold her arms down and keep her head straight, while the other did the actual application. We were instructed to change the whole get-up three times per day.

At this same appointment, we discovered that the particular type of NAM being used with Evie was experimental. Interestingly, this information wasn’t volunteered by the doctor, and only surfaced after I asked the orthodontist how long he had been doing it for. He admitted that he invented the device, is the only orthodontist in the world using it at this point, and it has only been used with a handful of other kids. Though NAM has been in existence a long time and used on kids with cleft palates with great success, this is the first NAM for kids with cleft lip only. This was news to us and we were a bit surprised, however, we figured there was no harm in trying it out.
After diligently attempting to do NAM for about five days, it became clear it was not going to work. It was difficult enough to get the device perfectly situated in the first place, and then over time as Evie nursed and the tape got wet and loosened, the device would inevitably shift and no longer be in the proper position. Since we were told it only needed to be changed two or three times a day, we thought we might be doing something wrong. Sean talked to a nurse about it, who said “oh yeah, that happens a lot”, we “just” need to change it after every time she breastfed. Um, what!?! When Sean told me what she said I literally laughed out loud. I don’t know if that nurse is aware of how often a newborn breastfeeds, but I certainly do not have the time or ability to perform a 20 minute treatment routine 8-12 times a day that requires two people when I have a husband who actually has a job, I don’t have a nanny, and I do have a (crazy) 2-year-old boy who I also have to take care of. Oh and did I mention they wanted us to return weekly for adjustments in Santa Clara, and the only available appointment time was on Friday afternoons? Between heavy traffic, the appointment itself, and stopping to nurse Evie, this was a six-hour round trip extravaganza. Believe me, it’s difficult enough to care for a newborn (and 2-year-old) without adding anything like that to the insanity!
After realizing it was completely unrealistic to continue with NAM, I still felt a great deal of guilt over discontinuing it, because as a mom, I obviously want to do everything I can to help my daughter. Part of me still wanted to make it work, but after discussing it with Sean and praying about it, we decided it was the right thing to do (although we have continued to do the lip taping, because we felt that was doable and actually effective). With the combined factors of the NAM treatment still being in the experimental phase, the inordinate investment of time, Evie’s hatred for the procedure, and our conscious rejection of the obsessive pursuit of physical perfection (in simple terms…we just didn’t think her nose was that bad), it became clear that it was not the right path for our family.
Tina, the orthodontist’s nurse, on the other hand, decided it was indeed the right path for our family, and made that very clear. LOL! But seriously. When we informed her of our decision, she literally yelled at us and accused us of not putting our daughter first and doing what was best for her. She told us no one else was experiencing the problems we were describing, and that we were giving up too soon (maybe they were too afraid to tell her)?? She also implied we were ungrateful for the orthodontist and his awesome treatment. So…that was an interesting experience.
On September 25th, when Evie was just shy of two months old, we took her to the craniofacial clinic at Kaiser Oakland. This clinic happens once per month and it was truly the mother of all doctor’s appointments – it was three hours long and she was seen by ten medical professionals: an ear/nose/throat doctor, head and neck surgeon, social worker, speech pathologist, nursing coordinator, medical assistant, geneticist, genetics counselor coordinator, orthodontist, and plastic surgeon. There were a number of other kids with clefts there (each in their own room), and the entire team of cleft specialists rotated through each patient’s room to do an examination and provide more information and resources. After all the kids were seen, the entire team met together to discuss each child and developed an individualized treatment plan. Although it was a long appointment, it was incredibly efficient and we were grateful to be seen by all these professionals at once. By the way…did you notice the orthodontist on the list of specialists? Yeah, that was kind of awkward.

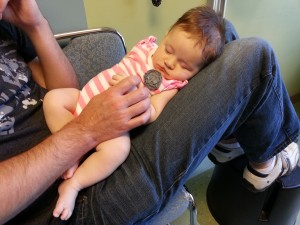
During this appointment, we learned from the geneticist that we have a 3-5% chance of having another child with a cleft, and Evie’s children will also have a 3-5% chance of being born with a cleft. He also confirmed that she does not have any syndromes associated with clefts. She’ll continue to be monitored by the craniofacial team through skeletal maturity at 16-17 years of age, and she may need (or rather, want) nose straightening surgery when her face is fully grown since her nostrils are asymmetrical (i.e. her nose is a little flat on one side). After her upcoming surgery on November 21st, her next group examination will be at two years old, when she will have a comprehensive speech and language evaluation, as well as a hearing evaluation from the team audiologist.

Although it is not anticipated that Evie will have any speech or hearing difficulties, we were told that some children with cleft lip only may have a submucous cleft palate, which means the skin covering the palate is intact and everything looks fine, but the muscles are not completely attached. The only way to detect this is by analyzing speech and resonance patterns after she starts talking. Also, since the palate muscles control opening and closing of the Eustachian tubes, her hearing will be monitored.
With Evie’s surgery just a few days away, it’s becoming more real that it’s actually happening. She will undergo general anesthesia (i.e. she’ll be fully asleep), and the surgeon will make an incision along the edges of her cleft lip extending up into her nose. She will then use stitches to bring the cut edges together to shape Evie’s upper lip and nostrils. Most children stay in the hospital for 1 or 2 days after surgery, and it usually takes about 3 to 4 weeks for the incision to fully heal. After surgery, it will be easier for Evie to nurse and breathe (and eventually, talk). The incision will leave a scar that will fade and become softer and flatter in the months and years after surgery. Since everyone heals differently, she may need an additional surgery around 5 years of age to address scar tissue.
The surgery will take approximately 2-3 hours, and we will not be able to see her until she wakes up. Immediately after surgery, she’ll be very groggy and probably won’t want to eat for a while. Evie’s particular surgeon allows breastfeeding right away (some surgeons require special bottles), so hopefully I will only need to pump four or five times before she returns to breastfeeding. However, from what I’ve read on an online cleft community group, I should expect her to have a difficult time breastfeeding for the first week post surgery since she will be groggy from painkillers, plus her lip will obviously be sore. It basically sounds like I should expect to nurse her all day long, since she will eat so slowly (I’m having flashbacks of newborn Caleb, ahhh)! She will also need to wear arm restraints (“no-no’s”) for two weeks to keep her hands away from her mouth and messing with her stitches. I think it will be difficult to see my sweet-natured, mellow baby girl experiencing such a hard time. Who knows though, maybe she’ll surprise me and her recovery won’t be as awful as I’m imagining, but I figure if I expect the worst, I can only be pleasantly surprised 🙂
In a strange way, I’m a bit sad to see her cleft go. I’ve become attached to her wide smile and it’s just uniquely her. Not a single person has made a rude or insensitive comment about it, which I’ve been thankful for (apparently lots of moms of cleft babies are asked what they did to cause it)!? How awful! I’ve also read online on cleft forums that there are some people, (usually dads), who want to abort after finding out their child has a cleft at the 20 week ultrasound, which absolutely breaks my heart. Maybe I’m sheltered or something, but that blows my mind that anyone would even consider killing their child over a purely physical problem like a cleft. Ugh! Anyways, I know we need to have Evie’s cleft repaired for medical reasons and not just for appearance, but I think she’s beautiful and perfect as is 🙂 Not to mention she has the sweetest little personality!

As we head into surgery, we’d really appreciate prayers for a smooth operation and recovery period. I would especially appreciate prayers for her to resume breastfeeding quickly and with relative ease, because I’m feeling anxious about that. Also pray for our family’s health – that none of us would get sick before or immediately after the surgery, since that would result in the surgery getting rescheduled (if she’s sick), or make it more difficult on us to care for her as she recovers (if we’re sick). It’s been an intense and busy few months, and I’m looking forward to getting past the surgery and for life to slow down and “normalize” a bit (whatever that means)!
So just in case this blog post wasn’t long enough for you (ha!), click here if you are interested in reading more about clefts!
And here’s a few more pics of Evie, plus a video, because I just can’t resist:

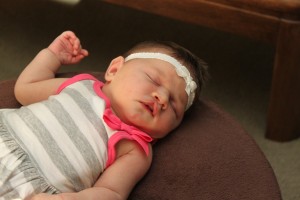




And just a few days ago, Evie laughing at 3.5 Months:
Evie’s Cleft Adventure Continues:
Evie’s Surgery Day Recap
First Day Post-Surgery Update
Second Day Post-Surgery Update
Third Day Post-Surgery Update
Fourth Day Post-Surgery Update
Fifth Day Post-Surgery Update
Days 6-10 Post-Surgery Update
3 Week Post-Surgery Update
1 Month Post-Surgery Update

I think you made the correct decision. Don’t let the doctors push you around. She is absolutely adorable! She looks a lot better. Andy and I will be praying for your entire family. Don’t fret about the nursing. If she’s hungry she will eat. I’m sure she will surprise you. If she loses a little weight she will pick it back up after she’s healed. If you hadn’t said anything about her nose I would not have noticed. My cousin had a very severe cleft palate when we were all little. Medicine has come a very long way! Again, bully for you for not letting that nurse push you around. Nobody knows what’s best for a child more than the mother. ♥♥♥
Awe love her laugh!♥
You two have the cutest babies!! 🙂 She is just a doll!
Not sure who your ortho was but we had issues with ours too and didn’t do the taping he wanted. It was unrealistic for us to d do, our some had a bad issue of projectile vomit after feeding and we would be changing it 3 or 4 times an hour.
Shaun and Melissa, Our daughter Hannah had a cleft lip and we waited to do surgery until she was nine months. As you might know, she is beautiful now and her scar is hardly noticeable. 🙂 God’s best to you guys!